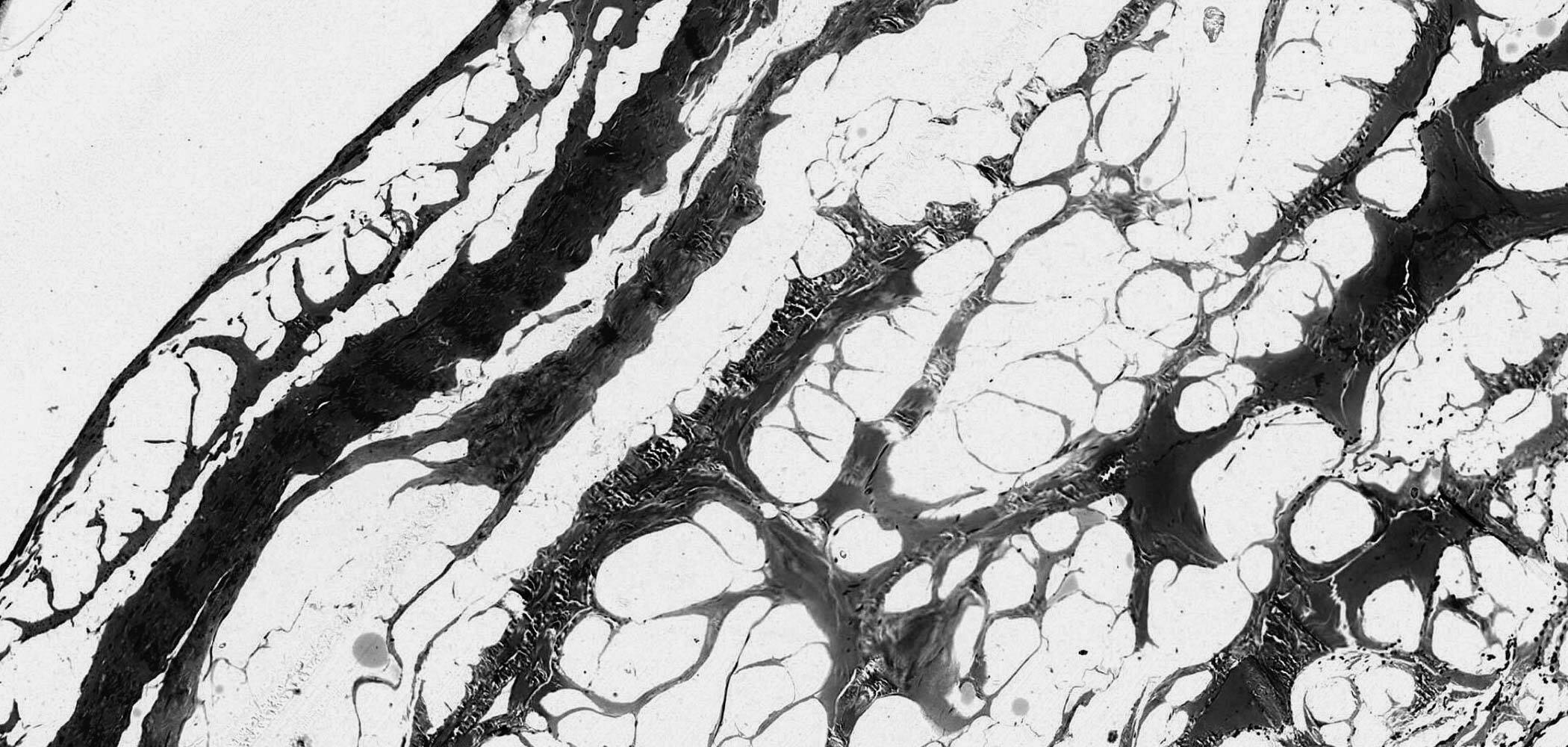
Bilayer:
the double layer that makes the difference
Bilayer bovine membrane
The Exaflex Bilayer bovine pericardium membrane is used in numerous medical disciplines that deal with the regeneration and repair of damaged tissues.
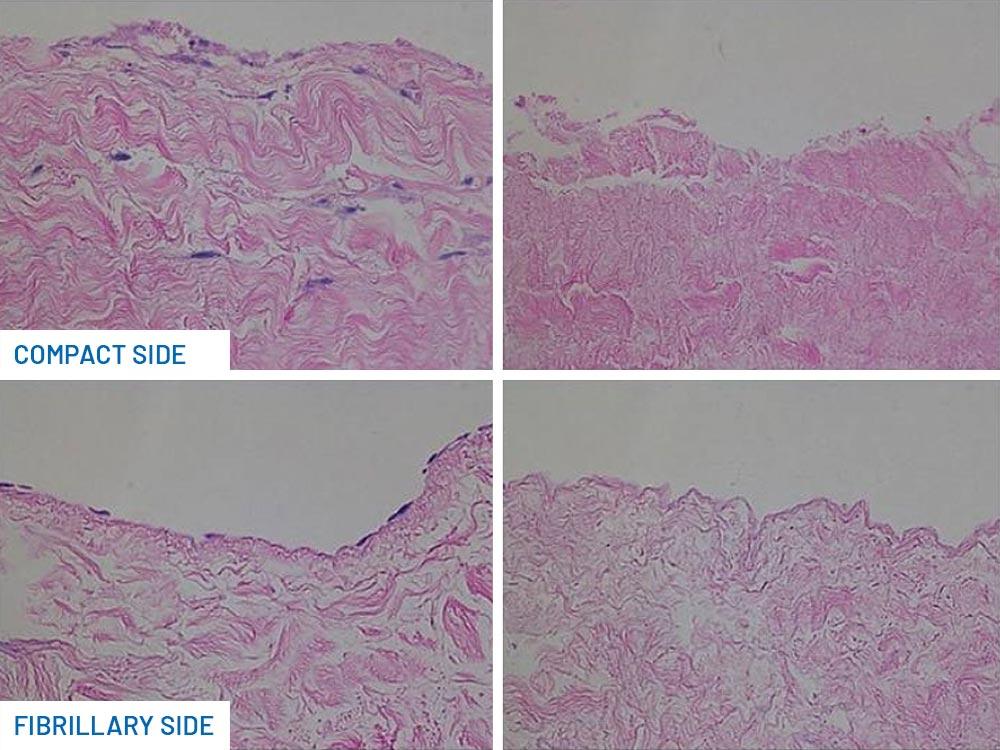
Exaflex consists of a double layer of multidirectional woven collagen fiber. One side is extremely compact, non-stick and very resistant to the passage of bacteria.
The other fibrillar side instead constitutes an ideal environment for the revitalization of the tissues, at the same time preventing unwanted movements of the prosthesis.
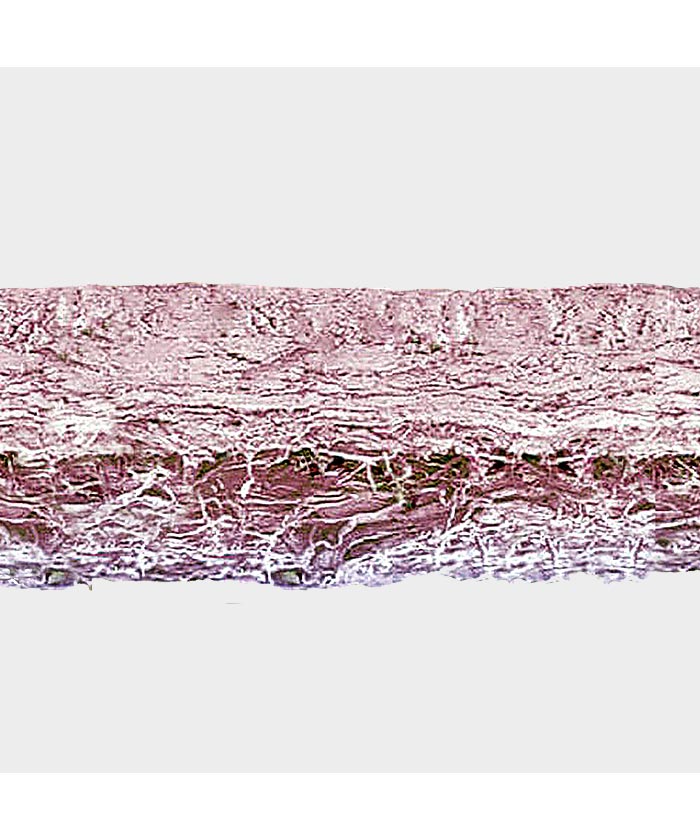
Compact and smooth, non stick layer

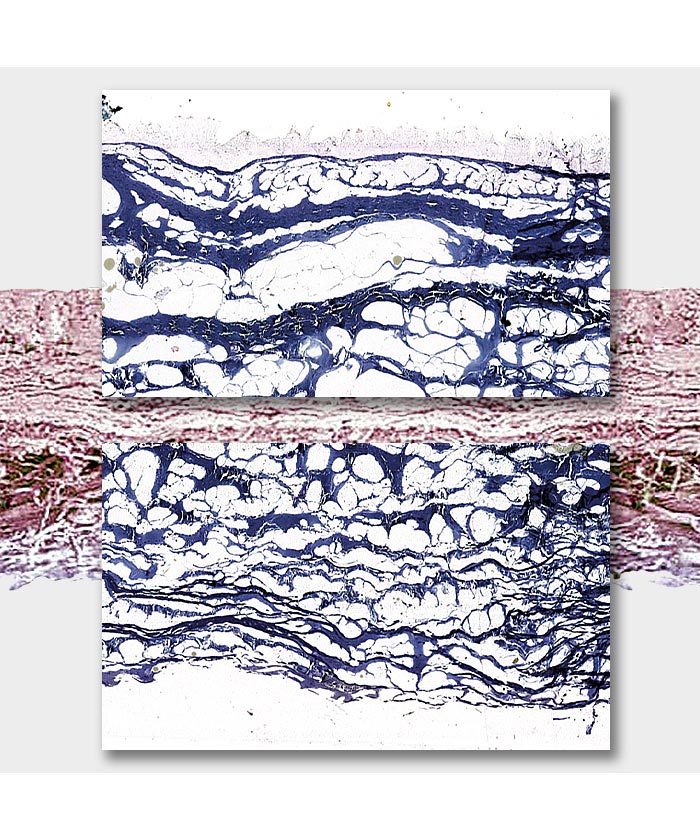

Fibrillar layer

Cross section of Exaflex membrane under electron microscope.
Anatomy Pathology - Hospital Città della Salute Torino.
Bilayer membranes undergo revitalization by endogenous connective tissue in 3 phases (phases of incorporation and absorption of a ADM):
- In the fibrillar layer the fibrocytes migrate and contribute to the anchoring of the membrane to the surrounding structures through the formation of a new membrane that surrounds the implant.
- The fibrocytes migrated into the three-dimensional structure of the bilayer membrane initially do not synthesize collagen but adapt their metabolism to contribute to the maintenance of the existing collagen fibers.
- After a few months, the degradation of the three-dimensional structure induced by the collagenases begins. The collagen is degraded and replaced by new fibrocytes. The neostructure is infiltrated and nourished by capillaries that grow easily in the three-dimensional matrix.
Thanks to its unique bilayer structure and pro-heal elements, the membrane guides the revitalization with the correct sequence of development of soft tissues and blood vessels, protecting the implants thanks to the compact layer.
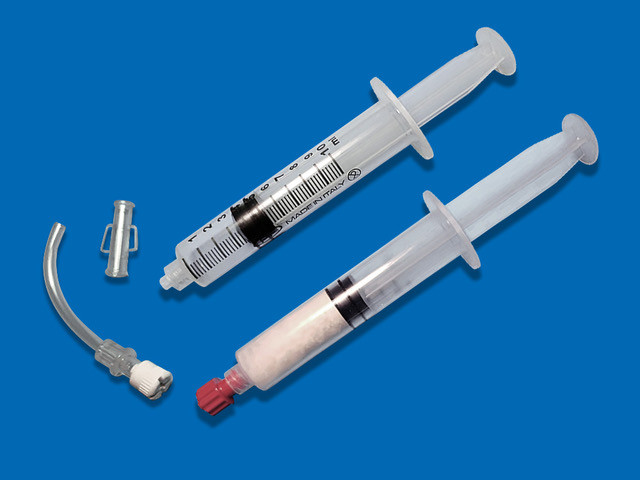
Processing procedure
The proprietary deantigenation process applied to Exaflex does not require acetone or ethanol and preserves all the regenerative active elements within the membrane.
Proteoglycans, hyaluronic acid, fibronectin, elastin and collagen provide a revitalizing reservoir, controlling inflammation and promoting cell proliferation and migration.
The amount of biological mass implanted is limited (up to 50% compared to dermal matrices) and integration is favoured, even in the case of poor perfusion, maintaining maximum biomechanical performance.
Componenti
Collagen
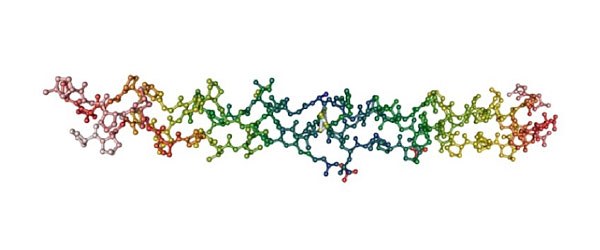
Main component of the membrane, made up of two layers: one compact and impermeable to external agents and one multidirectional, fibrillar, in contact with damaged tissues. The three-dimensional fibrillar layer is the ideal environment for cell settlement and vascular proliferation.
Elastin
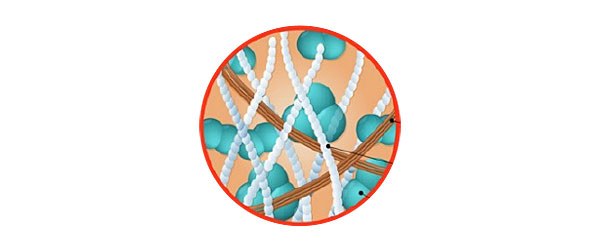
Connective tissue protein, found in abundance in the aorta and large blood vessels. Fundamental element of the skin, it makes the membrane extremely flexible and easily adaptable to the shape of the lesion.
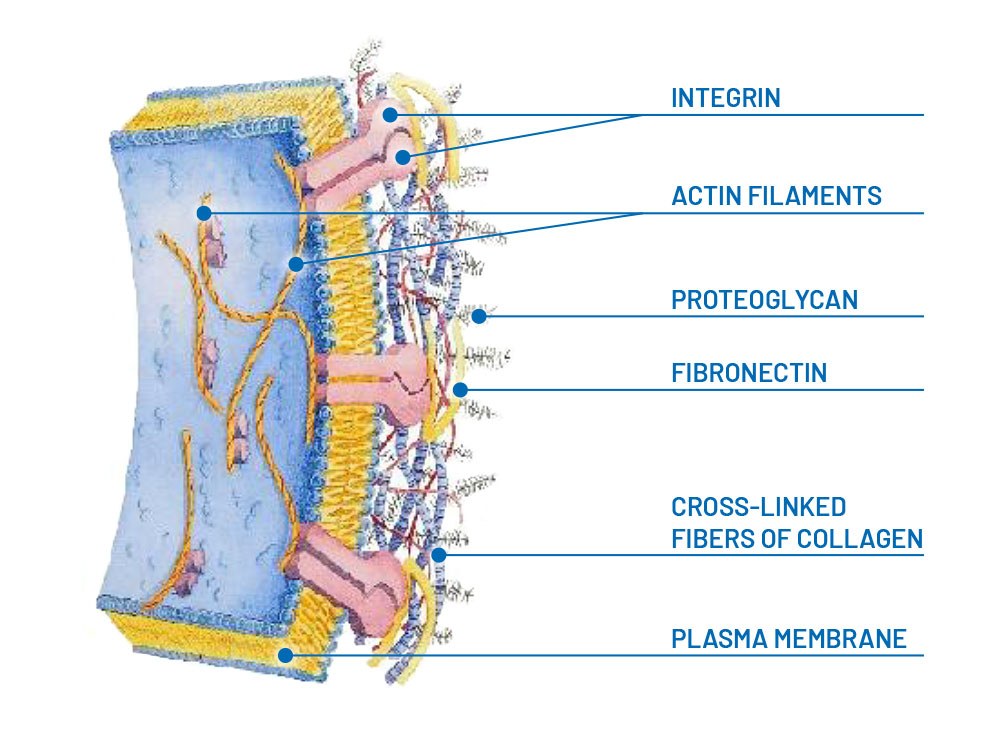
Fibronectin
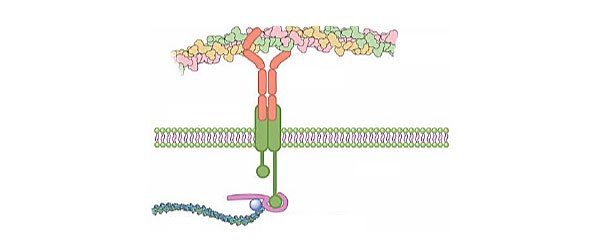
Protein that acts as a bridge between cells that need to attach to the extracellular matrix to move and collagen. Fibronectin dimers have two collagen binding sites and two membrane protein binding sites in cells: integrins. Cells adhere through this receptor to the collagen membrane which transmits signals to them.
Proteoglycans
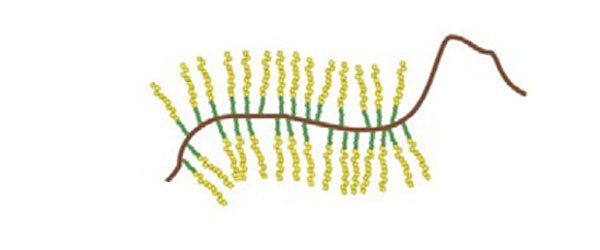
Components that "fill the spaces", guaranteeing resistance to compression. The glycosaminoglycan chains (thanks to their porous and hydrated organization) allow the rapid diffusion of water-soluble molecules and the migration of cells and their extensions.
Hyaluronic acid
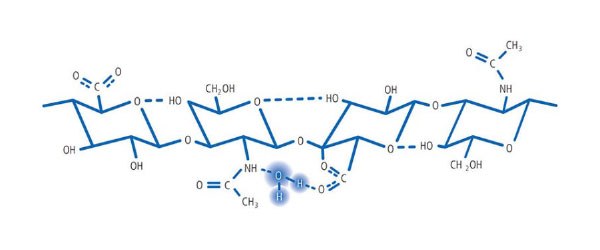
Its arrangement inside the scaffold allows it to occupy a high number of water molecules, maintaining hydration, plasticity and viscosity. Hyaluronic acid works as a filter against the spread of bacteria and infectious agents in the tissue. Only low molecular weight particles can pass through the "mesh" of this network and spread freely in the fabric.
Surgical applications
Acellular matrix products can be used in a wide range of applications, including burns and reconstructive surgery, soft tissue and abdominal wall repair, and as internal implants for orthopedic use in joint surface reconstruction and joint repair tendons.